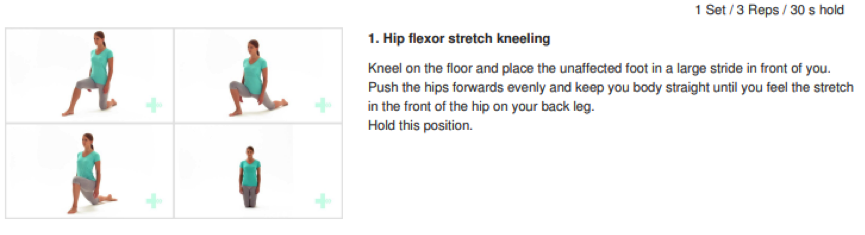
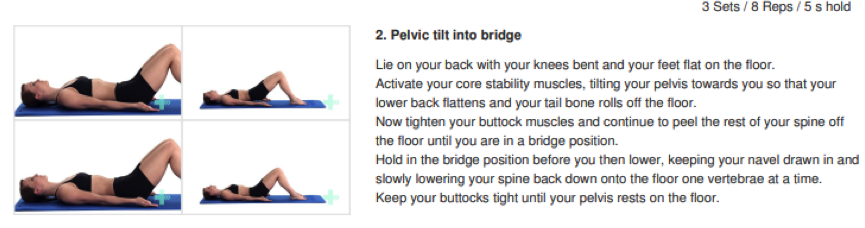
Ice and Heat for Musculoskeletal Injury Recovery
When should I use heat or ice for an injury?
Navigating at-home care for musculoskeletal injuries can be tricky, deciding when and when not to apply heat or ice can have a big impact – especially during the initial phase of an injury. R.I.C.E and H.A.R.M are useful acronyms for aiding the initial care of musculoskeletal injuries, but how do they work?
The principles of R.I.C.E and H.A.R.M can be applied for 3 days after the onset of an injury. During this period it is important to follow R.I.C.E – this stands for rest, ice, compression and elevation.
After applying R.I.C.E it is important to do no H.A.R.M – this stands for heat, alcohol, re-injury and massage. These are all things to typically avoid after a musculoskeletal injury.
R.I.C.E Principles:
Rest
The first component of RICE is rest. It’s essential to allow the injured area to heal by avoiding activities that may exacerbate the injury. Rest does not mean complete immobilisation; it simply involves minimising movement and avoiding activities that strain the injured area.
Ice
Ice therapy is a fundamental element in managing acute injuries. Applying ice helps reduce swelling and numbs the affected area, providing pain relief. The cold constricts blood vessels, limiting the amount of fluid that can accumulate around the injury site. Ice packs or cold compresses should be applied for about 15-20 minutes every 2-3 hours during the initial 72 hours after injury.
Compression
Compression helps control swelling by applying pressure to the injured area. Compression bandages or wraps are commonly used for this purpose. It’s crucial not to wrap the area too tightly, as this may impede blood circulation.
Elevation
Elevating the injured limb or area helps reduce swelling by allowing fluids to drain away from the injury site. Ideally, the injured area should be elevated above the level of the heart when possible.
H.A.R.M Principles:
Heat
Heat therapy is beneficial for chronic injuries or injuries that have moved past the initial acute phase. Applying heat increases blood flow, which in the acute phase can lead to more swelling. Heat should be avoided in the first 72 hours after an injury.
Alcohol
Alcohol, specifically excessive consumption, can impair the body’s natural healing process and should be avoided during the recovery period. Alcohol acts as a vasodilator, this means it will contribute to swelling especially during the acute phase. Alcohol can also interfere with medication, increase the risk of bleeding, and hinder the body’s ability to repair damaged tissues.
Re-injury
Avoiding re-injury is crucial for a successful recovery. Gradual reintroduction of activity should be guided by a healthcare professional. Rushing back into activities without proper healing increases the risk of exacerbating the injury.
Massage
Massage can be beneficial in the later stages of recovery. Similarly to heat, one of the main benefits of massage is increasing blood flow to the targeted area. In the initial phase however this can lead to further swelling and should be avoided, unless carried out by a healthcare professional.

Is heat always a bad thing?
Not always! Having explored the H.A.R.M principles, it’s essential to highlight the role of heat in the later stages of musculoskeletal injury recovery.
The first three days (or 72 hours) is known as the acute phase of an injury, after this period swelling should have peaked. As the acute phase subsides, heat becomes a valuable asset in promoting healing. Heat applications, such as heat packs or hot showers promote blood flow, which aids in delivering nutrient rich blood and oxygen to the injured area.